I work with affiliate advertising companies, which means if you click on or purchase a product through a link, I may earn a commission. However, all opinions remain my own...I promise!
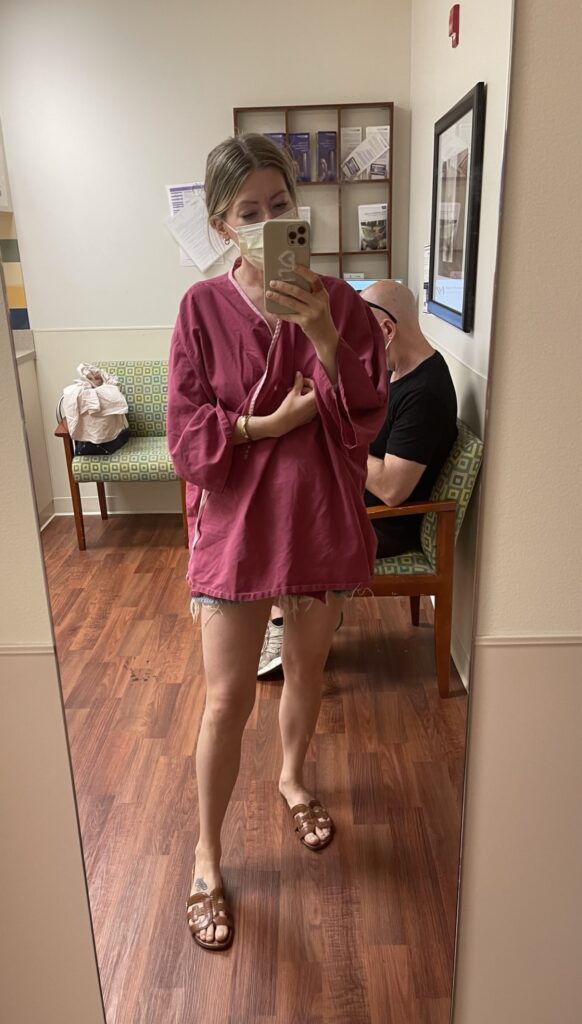
It’s hard to believe, but today marks 1 year since my unofficial breast cancer diagnosis, March 30, 2022. I write ‘unofficial’ because it was not the day my official biopsy results came back, but rather the day the doctor looked me square in the face and said “I’m sorry to tell you this, but I am 90% certain you have breast cancer”. Immediately I thought about my husband and 2 small kids. I was alone, terrified and felt like the room was caving in around me.
My story is not much different from the hundreds of thousands of other women’s stories who have been diagnosed – they find a lump, have a mammogram/ultrasound, get diagnosed and begin breast cancer treatment. In theory, the story line is so simplistic. In reality though, this story is completely life-altering, terrifying and sometimes (dare I write it) deadly. Each year in the United States, about 264,000 cases of breast cancer are diagnosed in women and about 2,400 in men. About 42,000 women and 500 men in the U.S. die each year from breast cancer.**
How It All Started
Just A Small Bump
One night in the Fall of 2021, just short of turning 39, I was sitting in bed watching tv and felt a small pea-sized bump on the far side of my left breast. It almost felt as if it were not on my breast at all, but rather on the side of my chest wall. Being a mom of two, I didn’t have much breast mass left after breastfeeding for just over 3 years (I’m sure some of you moms can relate). I sometimes think about why I was even touching the side of my breast and can only come to the conclusion that I might have had an itch or that it was mindless hand movement as I watched whatever show I was watching on tv. When I first felt the small bump, I wasn’t worried, concerned or panicked. I chalked it up to being a breast cyst since one year prior I was told I had a benign cyst on the far side of my left breast. I remember thinking that I had an upcoming annual OB appointment in early December and would bring it up to my doctor then.
Reschedule, Reschedule, Reschedule
Fast forward to early December – me and my entire family became sick with Covid. I had to cancel my appointment and reschedule to early February (the only opening they had). I wasn’t in a rush at that point since I still didn’t think much of the bump on my breast. In my mind, I had a benign cyst. Early February came around and once again, sickness plagued our household. This time my son was sick so I had to push my annual OB appointment once again. This time, to March 4th. At the appointment, my OB did her usual wellness checks on me along with a breast exam. When I pointed out the bump to her, I recall her feeling it and saying, “Hmmm. I’ll go ahead and order a mammogram and ultrasound to make sure it’s nothing”. I often wonder now if she had an inclination at the time but didn’t want to panic me.
In The Middle With Fear
My appointment at the Northwest Lynn Sage Breast Center consisted of a mammogram and ultrasound. Since I have extremely dense breasts, the ultrasound solidified my unofficial breast cancer diagnosis. My tumor could barely be seen on the mammogram images due to the density of my breasts. After the doctor delivered the news to me, I remember feeling as though I was in a dream. Reality didn’t make sense, so it had to be a dream. As the doctor left the ultrasound room, the kind technician stayed behind with me and did her best to comfort me. I recall her saying, “Maybe it’s just an ugly lymph node. Don’t give up hope”. I clung on to every word she said as I left the room. Soon after, I called my husband (in shock) to tell him I had breast cancer.
The Biopsy
The weeks that followed consisted of a biopsy, day-to-day life events, birthdays, a double breast MRI, doctors appointments, holidays and one set of genetic testing. The biopsy was somewhat traumatic – as the doctor and nurses called me into the procedure room, my legs felt like they weighed 500 pounds each. I was frozen and could barely muster the mental strength to get up from the waiting room chair and walk into the procedure room. Looking back, I think deep down I knew that there was no turning back after the procedure. I would know the exact diagnosis of my cancer, and mentally that was a load I was not ready to carry. The biopsy itself was a bit painful, and the ‘punch’ excision process was not something I was prepared for. I was also terrified the entire time. A kind doctor noticed tears rolling down my face and offered to hold my hand for the entire time of the procedure, and did just that. She was a Godsend. About five days after the biopsy, I received a call back from the doctor around 12:15 in the afternoon. I was officially diagnosed with stage 1, invasive ductal carcinoma. My tumor was 100% E/R+ and HER2-, and it measured .6cm. The Ki-67 marker was <10% and the p53 marker was <2%. Later on in my journey I would learn that these low percentages were in my favor.

MRI + Genetics Testing
Next came the breast MRI – praise God, it didn’t show any additional breast tumors nor did it show any enlarged lymph nodes. These were all signs that my cancer was isolated and not aggressively spreading. The next question became whether or not to remove my breasts entirely. Before I could make that decision, I was referred to a genetics counselor that would run genetics testing on my DNA. Once again, I received great news that the testing came back negative and did not identify any positive results or harmful variations in my DNA linked to increased cancer risk. Long story short, I could keep my breasts! My fear was starting to become more manageable and we now had a path forward based on this information.
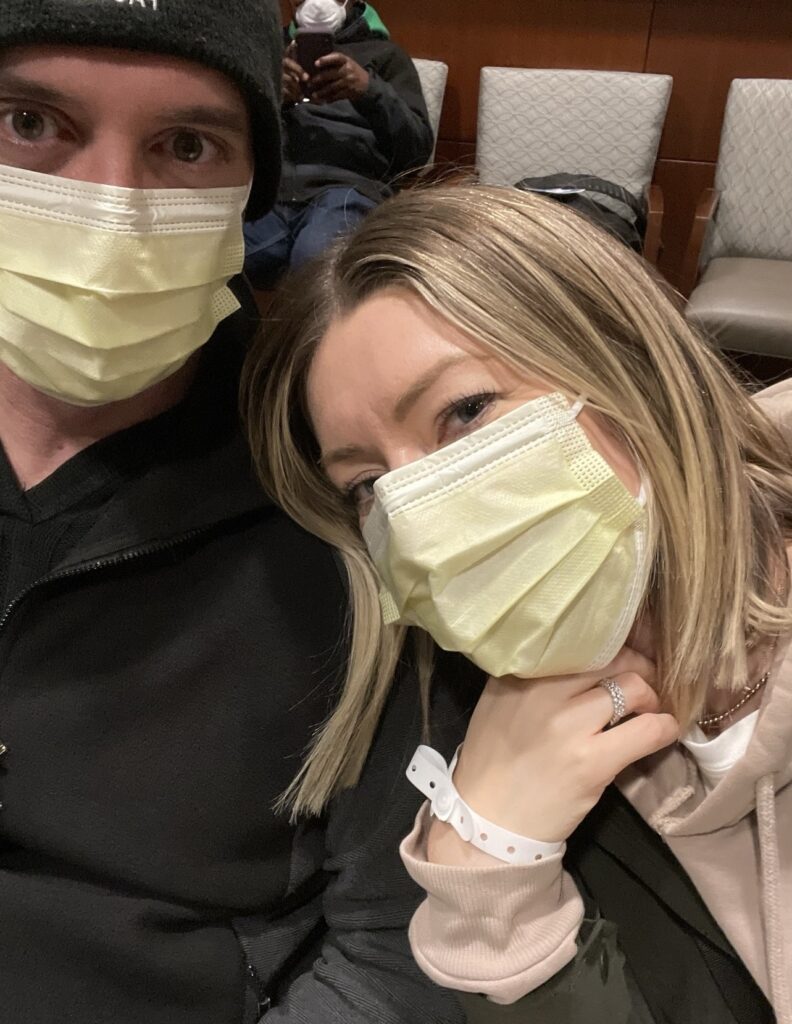

Lumpectomy
My lumpectomy surgery with node dissection took place on June 2nd at approximately 6AM in the morning. When someone is undergoing surgery for breast cancer removal, standard procedure is to also remove 4-5 lymph nodes to send to pathology. From there, it will be determined if the breast cancer has spread to the nodes. My sister and husband were with me, and interestingly enough, I wasn’t really nervous about it at all. I prayed for peace and calm leading up to the surgery, and believe God wholeheartedly answered me back. The surgery lasted just over 2 hours and I was discharged just as quickly as I was admitted. Several days later, the surgical pathology results came back. The tumor was measured at 1.6cm which was larger than originally measured in the biopsy. The pathology also showed that 2 of the 3 lymph nodes removed showed micrometistatic disease, with the largest carcinoma measuring .1cm. After my surgery, I was considered NED (no evidence of disease).

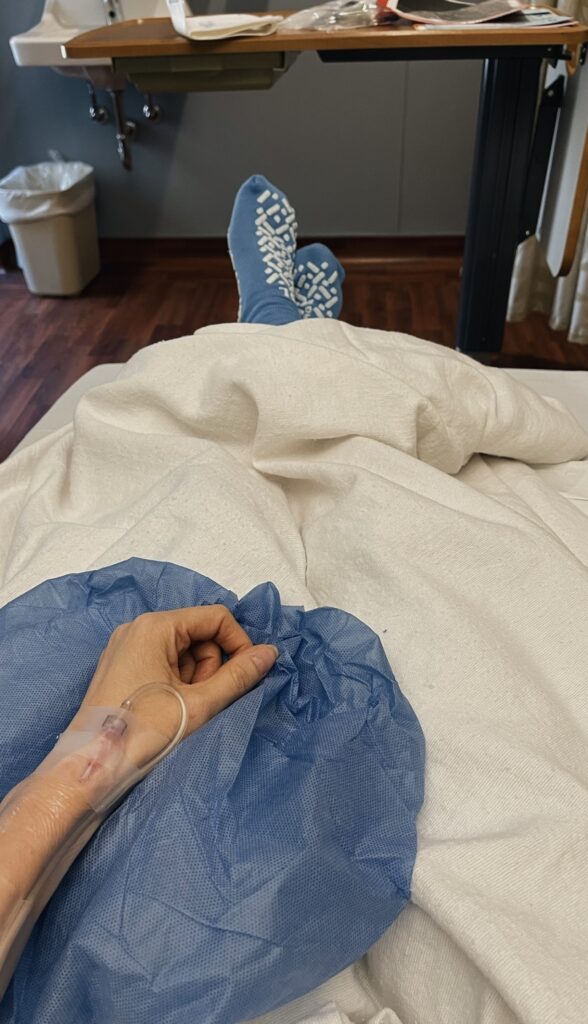
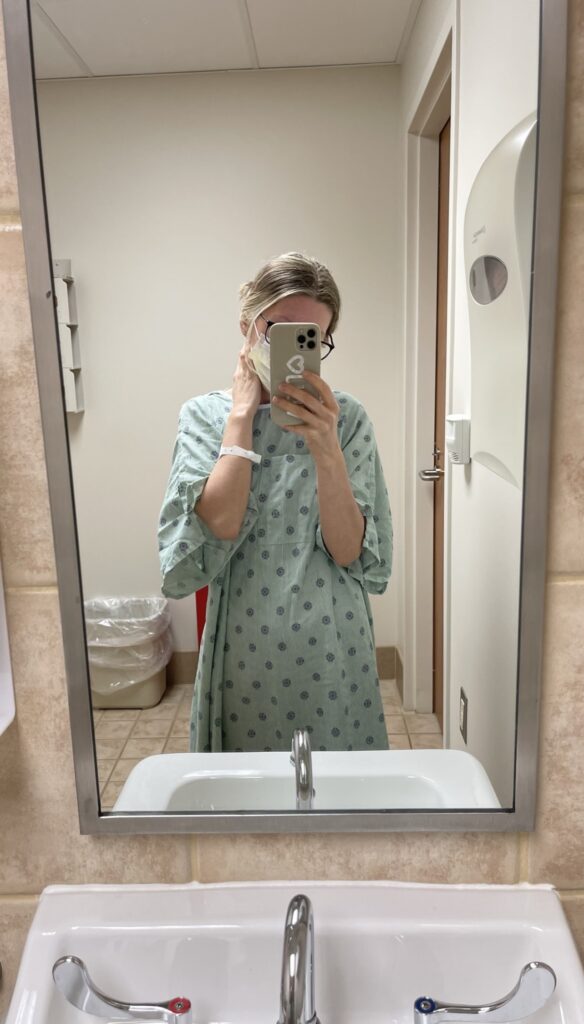
My Treatment Plan Minus The Chemo
I was shocked and scared to learn that my cancer was beginning to spread to my lymph nodes. I can only explain it by saying that I felt very let down by my own body. I was still hanging onto the great news of the clear breast MRI and negative genetics testing. Given the new pathology, the treatment conversation went from having a lumpectomy and radiation to lumpectomy, chemo and radiation, plus hormone meds. I knew very early on that I was not comfortable with chemo. At least not yet given I had micrometastatic disease (emphasis on the MICRO). To further support the path forward, I requested the Oncotype Dx testing be expedited to help figure out the plan forward. The Oncotype Dx test is a predictive gene expression test that attempts to predict the chances of your cancer returning. My score came back at 16 which is in the low recurrence range for premenopausal women with node negative pathology – no chemo is typically recommended; however, since I had micromets in 2 of the 3 nodes, that put me into a ‘gray’ category. It’s written that patients with node positive scores of 16-25 may benefit from chemo but it’s unclear if the benefit is really derived from hormone suppression alone. So, I voiced my thoughts and concerns to my oncology team and they were supportive of me having several weeks of radiation treatment plus hormone therapy alone.

Proton Radiation
Because my breast cancer was on my left side, the radiology oncology team recommended I have proton radiation instead of photon radiation. Proton therapy delivers a beam of proton particles that stops at the tumor, so it’s less likely to damage nearby healthy tissues and organs. Just days after Halloween, I completed 7ish weeks of daily radiation. My skin turned red, bled a bit and peeled off. If you or someone you know is undergoing radiation treatment, I HIGHLY recommend the Miaderm Radiation Relief Cream. My dermatologist recommended the cream to me and I believe it single-handedly was the reason why my skin recovered so quickly post treatment. Since treatment, I’ve noticed that my arm and shoulder area is tight and sore from the node dissection and radiation treatment. I’m currently undergoing acupuncture and (soon) physical therapy to help with the ‘cording’ and shoulder mobility issues. These are the things that are not talked about often enough after breast cancer treatment!
The handprints you see in the photos below belong to all of the children under the age of 18 who completed proton radiation therapy at the Northwest Medicine Proton Center. Proton radiation is the preferred method for young kids and babies since it’s less likely to damage nearby tissues and organs. I couldn’t help but be moved to tears when I saw these handprints on the walls. During the course of my treatment, I would often see 1 or 2 of the same young children (under 5) that were also getting treatment. They would be in their little hospital gowns and often sedated on a bed and being rolled into a treatment room. Children are put under local anesthesia for every treatment that only lasts 3-4 minutes. Their parents were always by their sides. I can’t imagine the strength it took the parents to go through that 5 days a week, for weeks on end.


Hormone Therapy
In January of 2023, I began taking Tamoxifen as part of my daily hormone treatment. Tamoxifen works by locking on to the estrogen receptors in the breast to block estrogen from attaching to them and therefore not allowing estrogen to fuel cancer growth. Most women are prescribed this medication anywhere from 2 to 5 years. More recently, it’s been recommended that ER+ cancer survivors stay on the medication for at least 10 years. Although I knew how important controlling the estrogen in my body was, the thought of putting a potentially toxic medication into my body put me into a place of great fear. According to the NIH, Tamoxifen is a known carcinogen with a long list of potentially harmful side effects. My decision to take this drug was not made lightly. So much so, I didn’t start taking the medication until 3 months or so after the first bottles were prescribed to me. The normal dosage for Tamoxifen is 20mg per day. Since I had a lot of concerns on how my body would react to the medication, I worked with my oncologist to prescribe me a 10mg Rx instead. For a month, I eased my way into the medication by taking 10mg each morning. After I felt comfortable that my body didn’t implode on the medicine, I began taking another 10mg at night to give me a total of 20mg per day. I still stick to this dosage and will continue to do so for the foreseeable future. If you have concerns or doubts on your prescribed dosage of hormone meds, talk to your oncologist. Being able to have that honest conversation made me feel like I was making the right decision for my cancer treatment. I was extremely nervous that the medication would wreck havoc on my body. To my surprise, I’m tolerating it really well so far. I haven’t had any hot flashes or notable side effects. I had some lower abdominal cramping in the first few weeks of taking the meds, but that has ceased now that I am almost 3 months in.
Where I’m At Today
Today, I’m happy to say that I am cancer-free and no longer living in fear. This hasn’t always been the case, though. For weeks following my radiation treatment, I lived in a state of anxiousness and fear. While I was in treatment, I had daily X-rays of my chest area along weekly monitoring by my oncologist. When you are no longer in treatment, it can play with your mind a bit. Am I still ok? Has the cancer returned? These are the questions that plagued me morning, noon and night. By the grace of God, I was reminded to leave my worry and anxiety to the Lord, and by doing so have experienced a sense of peace I’ve not known throughout this journey.
I know that the road ahead might present some challenges and I may have to be on medications for years to come, but I am optimistic about my future. Since my diagnosis, I have cleaned up my eating and beauty products, started taking a number of new supplements and vitamins, prioritized sleep and focused on eliminating as much stress as I could. I’ve seen two integrative doctors that I just love (more information on them in a separate blog post!) and have completed additional testing/blood work to get a better idea of my body’s ‘terrain’. I’ve also had my hormones tested since my breast cancer was fueled by estrogen. In addition to all of this, I’m getting acupuncture to help reduce stress and help with arm mobility and once a month seeing a therapist who specializes in cancer. My husband and I even purchased a low EMF infrared sauna for our home. As we all know, our bodies lay the foundation for our health, and I’m a big believer that mind, body and spirit play a huge role in one’s overall wellness. In addition to all of this, I’ve read numerous books on cancer. I wrote a blog post on my favorite cancer books that I really got a lot out of. You can read that blog post here. Next step will be getting high dose vitamin C infusions along with resveratrol infusions. I will be sharing my journey on that as well in the coming months.
My next hurdle comes on Friday, April 7th. That is the day I will be having my one year mammogram and ultrasound since diagnosis and treatment. I’m not really nervous (definitely not nervous like a year ago!), but I am looking forward to hearing that the results are clear and no cancer has been detected. I’ve already told myself that should something come back abnormal, I will praise God in that moment and pray for calmness in the storm of fear. I know He will sustain me. Update April 2023: My ultrasound and mammogram came back clear with the exception of a few small cysts in my right breast (the non-cancerous breast). Praise God!
If you or anyone you love is currently going through treatment for breast cancer or has been recently diagnosed, please know there is hope. If you got this far in reading my story, thank you. Writing my one-year journey has been cathartic, and I sincerely appreciate your readership. I can only hope that someone going through their own battle finds this blog post and knows they are never alone. “The Lord will fight for you; you need only to be still” -Exodus 14:14












